Case Study: Heel Pain from Plantar Fasciitis in 27 Year Old Male
Presentation: Plantar Fasciitis
A 27 year old male presented at the Sydney Heel Pain Clinic, experiencing heel pain in both feet and his symptoms were indicative of plantar fasciitis. The patient advised the sports podiatrist that his heel pain had been present for around 8 months that he could recall. He was overweight (BMI>30) but otherwise had no serious health concerns. He had a mostly sedentary lifestyle, working a desk job five days per week and enjoying video games on the weekends.
The patient and his girlfriend had recently adopted a new dog and had begun taking it for walks in the evenings, however the patient often experienced heel pain and it discouraged him to be active. His girlfriend encouraged him to visit the sports podiatrist for a correct diagnosis as she said it sounded like plantar fasciitis.
Patient’s Pain Symptoms: Consistent with Plantar Fasciitis
The patient described heel pain that was consistent with a diagnosis of plantar fasciitis. The patient described his pain as feeling like a stabbing at the base of his heel. His pain was very bad first thing in the morning as he got out of bed. It would subside and feel more like a dull aching after some time of moving around. During the day, he would feel the sharp heel pain again when he would rise from his desk chair after being seated for some time. On the occasions that the patient would walk his dog, his pain would return after he finished exercising. The sports podiatrist informed the patient that his heel pain symptoms were typical of plantar fasciitis.
Plantar Fasciitis Examination and Assessment
In order to confirm his suspicion of plantar fasciitis, the sports podiatrist carried out a thorough examination. He began with a comprehensive list of questions regarding the patient’s pain symptoms, medical history and physical activity habits. The sports podiatrist examined the patient’s feet. The range of motion and strength in the foot and ankle joint were assessed, as well as the flexibility of the patient’s lower leg and foot muscles, ligaments and tendons.
The patient was asked to have an ultrasound to aid the sports podiatrist diagnosis of plantar fasciitis, and to exclude any other injury or abnormality that may be causing the patient’s heel pain. He returned the following week with his results.
Biomechanical Assessment for Plantar Fasciitis
As part of the sport’s podiatrist’s assessment of the patient for plantar fasciitis, he carried out a biomechanical and gait analysis. The in-house treadmill at the clinic was used to perform this. The assessment involved placing some markers on the patient’s lower leg and foot and then recording footage of the patient walking on the treadmill. The sports podiatrist was then able to review the patient’s foot strike in slow motion and detect malalignment or functional abnormalities. Heel angle and foot arch height in the patient’s feet were also measured.
Biomechanical Assessment for Plantar Fasciitis
As part of the sport’s podiatrist’s assessment of the patient for plantar fasciitis, he carried out a biomechanical and gait analysis. The in-house treadmill at the clinic was used to perform this. The assessment involved placing some markers on the patient’s lower leg and foot and then recording footage of the patient walking on the treadmill. The sports podiatrist was then able to review the patient’s foot strike in slow motion and detect malalignment or functional abnormalities. Heel angle and foot arch height in the patient’s feet were also measured.
Notable findings of the examination for plantar fasciitis
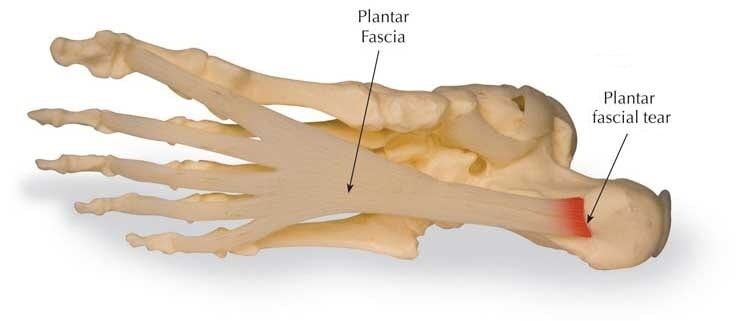
- The patient reported strong pain when the sports podiatrist applied pressure to the plantar aspect of the heel (the approximate location where the plantar fascia ligament connects to the heel bone)
- The patient had poor flexibility in his calf muscles
- The patient exhibited pes planus (fallen arches)
- During the biomechanical assessment, the patient exhibited increased foot width and it was determined that there was peak pressure from weight bearing during walking under the longitudinal arch
- The patient had increased plantar fascia thickness (4.9mm), evident on the ultrasound, confirming a case of plantar fasciitis.
Diagnosis Confirmed: Plantar Fasciitis
The sports podiatrist informed the patient that he had plantar fasciitis: inflammation of the plantar fascia ligament due to chronic overuse.
Treatment for Plantar Fasciitis
Once the patient’s plantar fasciitis diagnosis was confirmed, treatment could begin. The main goal of the treatment for his heel pain was to reduce strain on the plantar fascia and relieve the patient’s pain, while at the same time, allowing the plantar fascia to heal.
The recommended treatment plan comprised five main components:
- Stretching the patient’s tight calf muscles
- Taping for plantar fasciitis
- Custom shoe inserts
- Shockwave therapy
- Weight loss.
The sports podiatrist demonstrated to the patient which exercises he should perform to help increase flexibility in his calves, which would reduce the strain on the plantar fascia. The patient was instructed to carry out his stretches three times daily, especially before bed.
The sports podiatrist also instructed the patient on how to strap his feet in a way that would support his arches and unload the plantar fascia, providing pain relief and allowing it to heal. Custom shoe inserts were arranged for the patient. The sports podiatrist explained that the custom orthotics the patient would receive would touch and hold the sole of the foot, unloading the plantar fascia and allowing it to heal. The sports podiatrist recommended that the patient should wear his custom orthotics on a daily basis for 6-8 weeks. This would help to relieve his pain in the short term but also allow the plantar fascia to heal in the longer term.
Shockwave therapy was recommended for this patient’s plantar fasciitis treatment. It is an evidence-based treatment for the condition. It has the potential to offer the patient instantaneous pain relief. Shockwave therapy works by stimulating tissue regeneration and encouraging blood flow to the injured or inflamed area. The patient received four shockwave therapy treatments over the course of four weeks.
The sports podiatrist discussed maintaining a healthy body weight with the patient. He encouraged his patient to try to lose some weight, as extra bodyweight puts a lot pressure on the structures in the feet, often causing foot and heel pain. Scientific studies have shown a statistically significant relationship between increased BMI (body mass index), fat mass, and foot pain2. Further studies also demonstrated that patients with chronic plantar heel pain were almost three times more likely to have a BMI of 30 or more1. A change in diet was suggested and the patient was provided with resources for nutrition information. The patient was also advised to begin some low impact exercise (swimming was advised) while his plantar fasciitis healed, until he would be able to walk briskly with his partner and their dog again.
Plantar Fasciitis Treatment Outcomes
The patient completed his course of shockwave therapy treatments for his plantar fasciitis. He reported an immediate reduction in pain on all occasions.
He had been diligent in completing his prescribed exercises. The sports podiatrist advised his patient that he should continue to perform these in the long term so that he could maintain his flexibility, and for general wellbeing. The patient reported that he found his orthotics comfortable, and that they seemed to be providing him with support in the right places and helping with his pain.
The patient returned for his final check up twelve weeks after his initial visit to the clinic. He reported to his sports podiatrist that on most days he was completely pain free. At that point in time, he was wearing his orthotics on most days thorough the week, and continuing to complete his stretches on a daily basis. The patient had been swimming twice a week and he had begun incorporating walking into his exercise regime three times a week. He had managed to lose a reasonable amount of weight in that time too, which was no doubt helping him to feel better overall.
Please be advised that this case study is unique to this individual patient. Any treatment details mentioned are not intended, nor should they be taken as general medical advice. If you are experiencing heel pain or suspect you might have plantar fasciitis, you should make an appointment with a qualified sports podiatrist for a correct diagnosis and treatment plan.
Podiatrist – Omar Mohamad
Sydney Heel Pain Clinic – North Sydney
93883322
References:
1Irving, D.B., Cook, J.L., Young, M.A., Menz, H.B., 2007, Obesity and pronated foot type may increase the risk of chronic plantar heel pain: a matched case-control study, BMC Musculoskeletal Disorders, 8, 41.
2Tanamas, S.K., Wluka, A.E., Berry, P., Menz, H.P, Strauss, B. J., Davies-Tuck, M., Proietto, J., Dixon, J. B., Jones, G., Cicuttini, F.M., 2012, Relationship between obesity and foot pain and its association with fat mass, fat distribution, and muscle mass. Arthritis Care Research, 64, 262-268.
Written by Karl Lockett



